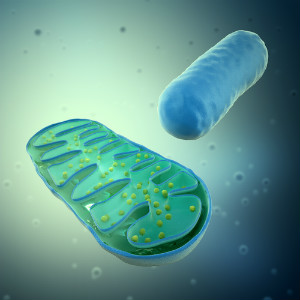
Mitochondria 101
Mitochondria (bacterial partners that came on board more than a billion years ago) are the powerhouses of the human cell. They convert the energy stored in sugars and fats into ATP, the essential energy molecule of all animals. Every muscle cell is filled with mitochondria, cheerfully combining sugars or fats with oxygen to yield water and ATP. Heart muscle and active neurons have the greatest concentration of mitochondria — as many as 5,000 per cell. Every day, your body’s mitochondria produce about 300 pounds of ATP to power both brain and muscle. Of course, there isn’t 300 pounds of ATP in the human body - when ATP gives up its energy to make a muscle contract, it reverts to ADP (a precursor molecule) and must then return to the mitochondria to be recycled into ATP. Each ATP molecule is recycled thousands of times per day.
Mitochondrial Defects and Disease
The Superoxide Dilemma
Much like the bacteria they come from, mitochondria also grow and divide. But they are not excessively independent. Their growth and the number of copies per cell is controlled by the cell nucleus, which also provides a good fraction of the protein building blocks that mitochondria need for growth. If a cell is running low on ATP, the nucleus senses this and orders up more mitochondria.
So far, this sounds like a happy relationship. But this “workhorse” organelle is subject to a lot of wear and tear, and they handle some dangerous chemicals as well.
When electrons from sugar and fat are combined with oxygen in the manufacture of ATP, reactive and potentially destructive forms of oxygen, known as free radicals or superoxides, are formed inside. These superoxides are normally neutralized by a specialized enzyme present throughout the organelle, known as superoxide dismutase. However, when this enzyme is defective or in short supply, superoxides can roam the cell and damage the mitochondria and other structures. This type of damage seems to be the explanation for the destruction of motor neurons in ALS, or Lou Gehrig’s disease, a paralytic disease with very poor prognosis.
Aging and Heart Failure
Even when all the elements of the mitochondria are working properly, the wear and tear from processing millions of reactive molecules every day can take its toll. As we age, mitochondrial DNA accumulates mutations and deletions. DNA synthesis slows or even stops, and the mitochondria may eventually be destroyed. At intermediate stages, they divide more slowly and make defective proteins that degrade their membrane functions. The membranes, which contain essential enzymes and electron carriers like coenzyme Q10 and cytochrome oxidase, begin to lose their integrity, and production of ATP becomes inefficient.
Cells can compensate somewhat for this aging phenomenon by calling for more mitochondria; indeed, the number of mitochondria per cell increases several fold in aging cells. But finally, in some tissues, such as heart and brain tissues, the mighty organelle may not be able to supply adequate amounts of ATP, and the organ begins to fail. Mitochondrial aging may be involved in memory loss and seems also to play a role in the dementia of Alzheimer’s disease. Similarly, chronic heart failure results in part from the inability of heart-muscle mitochondria to supply the ATP needed for muscular contraction.
Fighting Back with Antioxidants
It may be possible to prevent or ameliorate some mitochondrial damage by suppressing the damaging effects of free-radical oxygen. Investigators and nutritionists are pinning their hopes on antioxidant molecules like vitamin E, vitamin C, and coenzyme Q10. These molecules are a naturally occurring part of everyone’s diet, but they may also be taken as supplements. They can serve as a sort of molecular sponge for the reactive oxygen molecules produced throughout the body.
Vitamin E and coenzyme Q10 are particularly interesting, because both are highly soluble in lipids and therefore in cell membranes, where oxidative damage is often concentrated. Their presence in cell membranes may help limit damage to these structures by free radicals. There is good evidence that the two taken together as supplements can reduce the oxidation of low-density lipoproteins (LDLs) circulating in the blood. Oxidized LDLs are known to be involved in the development of atherosclerosis, or hardening of the arteries.
Coenzyme Q to the Rescue
Coenzyme Q10 (CoQ10), or ubiquinone, has shown promise in slowing or postponing diseases of the heart muscle itself, especially in advanced heart failure. In heart failure, the ability of the heart muscle to do the necessary amount of work is restricted by a defective energy supply, perhaps due to lack of substrates or essential cofactors. CoQ10, a natural coenzyme, plays a key role in oxidative phosphorylation, the ultimate source of the heart’s energy.
In one large Swedish study, patients with advanced heart failure were found to have lower levels of coenzyme Q than subjects with mild degrees of heart failure. In an attempt to restore normal levels, investigators supplemented patients’ diets with 100 milligrams of this coenzyme per day. They found that patients treated with coQ10 experienced beneficial effects on clinical outcome, physical activity, and quality of life, compared to patients treated with a placebo.
Other studies have demonstrated positive effects on parameters such as cardiac stroke volume, a measure of the efficiency of heart function. Although additional studies are needed, coenzyme Q appears to benefit patients who have failing hearts, with no measurable side effects. Coenzyme Q can also inhibit clotting, and this may be one of the mechanisms by which it improves cardiovascular functioning in chronic heart failure. In fact, a recent study has shown significantly reduced mortality rates in heart failure patients via CoQ10.
When coenzyme Q is taken orally as a tablet, powder-filled capsule, or as an oil suspension or solution in softgels, it is poorly absorbed and only a small percentage finds its way into the blood plasma. This low “bioavailability” of oral CoQ10 was found to be related to the dissolution rate of the formulation 1. The development of a hydrosoluble coenzyme Q10 (Q-Gel) dosage form has provided a highly bioavailable oral CoQ10 supplement, which facilitates up to 300 percent higher plasma Q levels over conventional oral supplements 2,3,4.
If damage from free radicals does produce accumulated mutations in mitochondrial DNA and thus speeds aging, then blocking this damage should slow aging and the onset of age-related diseases. Damage control might consist of lifelong treatment with antioxidant molecules, as suggested above.
REFERENCES
- Biomedical and clinical aspects of coenzyme Q, vol. 4, Elsevier, Amsterdam, 1984, pp. 131-142.
- FASEB Journal, 11:A586, 1997.
- Journal of the American Pharmaceutical Association, vol. 38, No. 2, p. 262.
- International Journal for Vitamin and Nutrition research, 68 (1998) p. 109-113.